Understanding the Care Gap for Long-Term Survivors of Breast Cancer
For many, the five-year mark after a breast cancer diagnosis represents a beacon of hope. It’s often celebrated as a milestone of survival. Yet for some, this pivotal moment transforms into an overwhelming void—an emotional landscape of uncertainty as they find themselves adrift in the murky waters of post-treatment life. Helen Carter, a 53-year-old breast cancer survivor from Ohio, recalls her journey with haunting clarity: “Once I rang the bell at my oncologist’s office, I felt a mix of relief and dread. No one told me what came next. It felt like falling off a cliff into a darkness I wasn’t prepared for.”
The Absence of Clear Guidelines
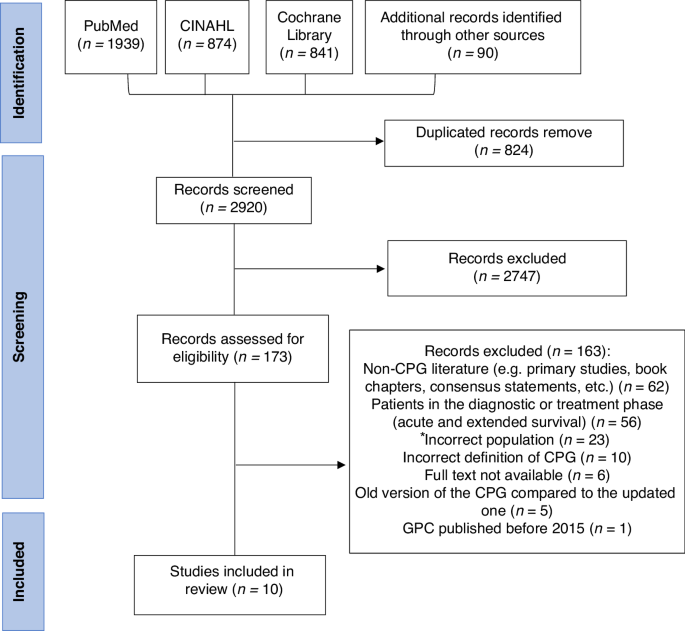
Recent research exposes a glaring oversight in oncology: the lack of clinical practice guidelines (CPGs) tailored specifically for long-term breast cancer survivors—those who have surpassed the crucial five-year period post-treatment. According to a systematic review published in the Journal of Cancer Survivorship, only ten guidelines provide any recommendations for this neglected demographic. This gap showcases a profound deficiency in addressing the ongoing needs of these individuals, who often grapple with lingering health issues and emotional ramifications.
“The existing CPGs predominantly focus on acute and short-term survivorship,” asserts Dr. Lisa Raynor, an oncologist at the National Cancer Institute. “This leads to a major oversight of the unique challenges faced by long-term survivors, including monitoring for recurrence and managing chronic health problems.” The review highlights the stark reality: guidelines for survivors beyond five years are alarmingly scant, leaving them feeling lost in transition.
Challenges in Transitioning Care
The transition from specialized oncology care to primary care can be fraught with challenges. Many survivors, once discharged from oncological programs, find themselves navigating a new healthcare landscape without proper guidance. Dr. Samuel Lee, a psychologist specializing in cancer recovery, notes, “This ‘lost in transition’ phase leaves many survivors without the support they need, contributing to feelings of helplessness and frustration.”
- Lack of Communication: Critical information regarding long-term care is often inadequately communicated to primary care providers.
- Limited Knowledge: General practitioners may not be sufficiently informed about the specific needs of cancer survivors.
- Emotional Distress: Survivors frequently face anxiety and depression during this transition, compounding their struggles.
This deficiency raises concerns about the quality of care, with numerous studies suggesting that inadequate management of post-cancer care can lead to poorer health outcomes. In fact, research published in the American Journal of Managed Care indicates that survivors without structured follow-up care report higher instances of psychosocial distress and physical ailments.
Filling the Gaps in Care
While some guidelines have touched on vital aspects such as surveillance and prevention, they largely ignore broader categories essential to holistic care. For instance, recommendations on lifestyle modifications—ranging from diet changes to exercise—are either vague or entirely absent. Dr. Maria Chen, a nutritionist specializing in cancer prevention, comments, “We know that lifestyle choices can drastically impact long-term outcomes for survivors, yet our guidelines lack the nuance necessary to support these patients.”
Recommendations for Improvement
To address these deficiencies, experts argue for the development of comprehensive guidelines specifically aimed at long-term survivors. Key areas of focus should include:
- Defined follow-up protocols and the frequency of necessary screenings.
- Guidance on managing late effects of treatments such as lymphedema and osteoporosis.
- Interventions targeting psychological well-being, including support for anxiety and depression.
- Recommendations for lifestyle changes that incorporate exercise, nutrition, and smoking cessation.
“By creating guidelines that incorporate these elements,” notes Dr. Raynor, “we can better support the needs of breast cancer survivors in a way that truly promotes their long-term health and quality of life.”
Charting a New Course
The journey toward improved care for long-term survivors necessitates collaboration between oncologists, primary care physicians, and the survivors themselves. By fostering this holistic approach, we can create a more robust framework for survivorship care. Respected figures in the field of oncology stress that integrating patient voices into the guideline development process is crucial. “Survivors have unique insights into their needs,” emphasizes Dr. Lee, “and their experiences should guide practice recommendations.”
To those like Helen Carter, the prospect of comprehensive, clear guidelines for long-term care would transform their journey. “After battling cancer, we shouldn’t have to fight for clarity in our health care,” she remarks. “Every survivor deserves to have a roadmap that guides them through life after treatment.”
As the medical community awakens to the needs of long-term breast cancer survivors, the path forward is clear: the creation of nuanced, evidence-based guidelines tailored to this vital stage of care not only promises to fill prevalent gaps but also to honor the resilience of those who have fought bravely against a difficult diagnosis.
Source: www.nature.com