Cardiometabolic Diseases and Cognitive Decline: A Dual Threat
As urban landscapes swirl with smog and a population ages, the alarming nexus between cardiometabolic diseases (CMDs) and cognitive decline unfolds in ways that demand urgent attention. Among 438,681 participants in a comprehensive study, 75,056 individuals, or 17.11%, were found to have CMDs. This alarming statistic becomes even more troubling when we consider that patients with one, two, or three of these diseases face a significantly heightened risk of cognitive impairments and various forms of dementia.
Demographic Insights: The Baseline Characteristics
Table 1 presents a stark portrait of the participants. Of those with CMDs:
- Age and Gender: The affected population was predominantly older and male.
- Employment Status: A higher proportion were retirees.
- Education and Economic Status: They tended to possess lower educational qualifications and poorer economic conditions.
- Health Metrics: The group exhibited lower normal BMI rates, increased dyslipidemia and hypertriglyceridemia, and higher usage of lipid-lowering medications and aspirin.
- Vitamin D Levels: A significant number experienced moderate to severe serum 25(OH)D deficiency, alongside hypertension.
- Psychological Factors: Interestingly, a lower prevalence of depression was noted among this group.
Experts urge caution in interpreting these findings. Dr. Helena Bergström, a leading researcher in public health, asserts, “The alarming trends we are observing indicate not only a healthcare crisis but a clarion call for policy intervention on lifestyle and environmental health.”
Interplay of CMDs and Cognitive Impairment
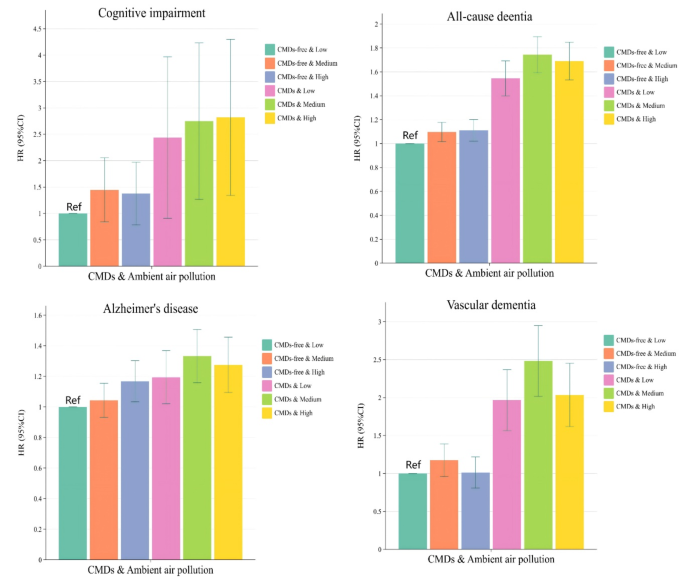
The risk of developing mild cognitive impairment, all-cause dementia, Alzheimer’s disease, and vascular dementia in those with CMDs was significantly higher: 1.951, 1.554, 1.216, and 2.032 times respectively when compared to those without CMDs. This poses serious implications, as those with multiple CMDs face even greater susceptibility to cognitive decline.
“Understanding the connections between physical and cognitive health is essential,” explains Dr. Raj Patel, a neurologist specializing in dementia care. “Cardiometabolic health is not an island; it influences every facet of well-being.”
The Role of Ambient Air Pollution
One of the study’s most compelling findings concerns the synergy between CMDs and ambient air pollution. When controlling for CMD status and pollution levels, research indicated alarming correlations:
- Patients with CMDs under high pollution exposure had a 2.562 times higher risk for mild cognitive impairment.
- For all-cause dementia, the risk rose to 1.686 times, for Alzheimer’s disease it reached 1.267 times, and for vascular dementia, 2.006 times.
This sharply illustrates the dual threat of environmental risk factors and long-term health conditions. According to the research, exposure to PM2.5 and other particulate matter has a particularly deleterious effect on cognitive functioning. “If you consider that air pollution is a daily reality for millions, the implications are profound,” Dr. Bergström adds.
Healthy Lifestyles: A Beacon of Hope
Interestingly, the study uncovered a glimmer of hope: the protective effect of leading a healthy lifestyle. Among participants who maintained healthy lifestyle scores:
- The risk for all-cause dementia, Alzheimer’s, and vascular dementia dropped significantly.
- Those with healthier scores (5–7) faced lower risks for cognitive impairment than their counterparts scoring lower (0–1).
“A healthy lifestyle acts as a buffer against the onslaught of chronic health conditions impacting cognitive function,” claims Dr. Patel. “Simple dietary changes, regular physical activity, and social engagement can make a difference.”
Complex Interactions: Pollution, Lifestyle, and CMDs
The interaction between ambient air pollution and lifestyle factors revealed a complex narrative. In CMD patients exposed to high air pollution and possessing low lifestyle scores, the risk of developing dementia soared. Conversely, healthier lifestyle choices seem to ameliorate some of the risks attributed to pollution. This interaction suggests that improving lifestyle factors could play a crucial role in mitigating cognitive decline, even in the context of CMDs.
Figures from the study illustrate a stark reality: the highest risk for dementia is found in CMD patients who are also burdened by poor environmental conditions. Dr. Patel vehemently argues, “The way forward must involve community-level policy changes to improve air quality, alongside advocating for healthier lifestyle choices.”
The data serve as a sobering reminder of the interconnectedness of modern life’s physical, social, and environmental circumstances. As urban centers grow, the implications of this research extend far beyond individual health; they call for a cohesive approach to public health that intertwines medical care, environmental policy, and community education.
As we confront the challenges posed by an aging population and escalating rates of CMDs, there is an urgent need for a comprehensive, multi-sectoral response. By understanding the profound interplay of cardiometabolic health, cognitive decline, and environmental factors, we carve a path toward a more healthy future—one where informed policy and proactive community initiatives lead the charge against the looming specter of cognitive impairment.
Source: www.nature.com