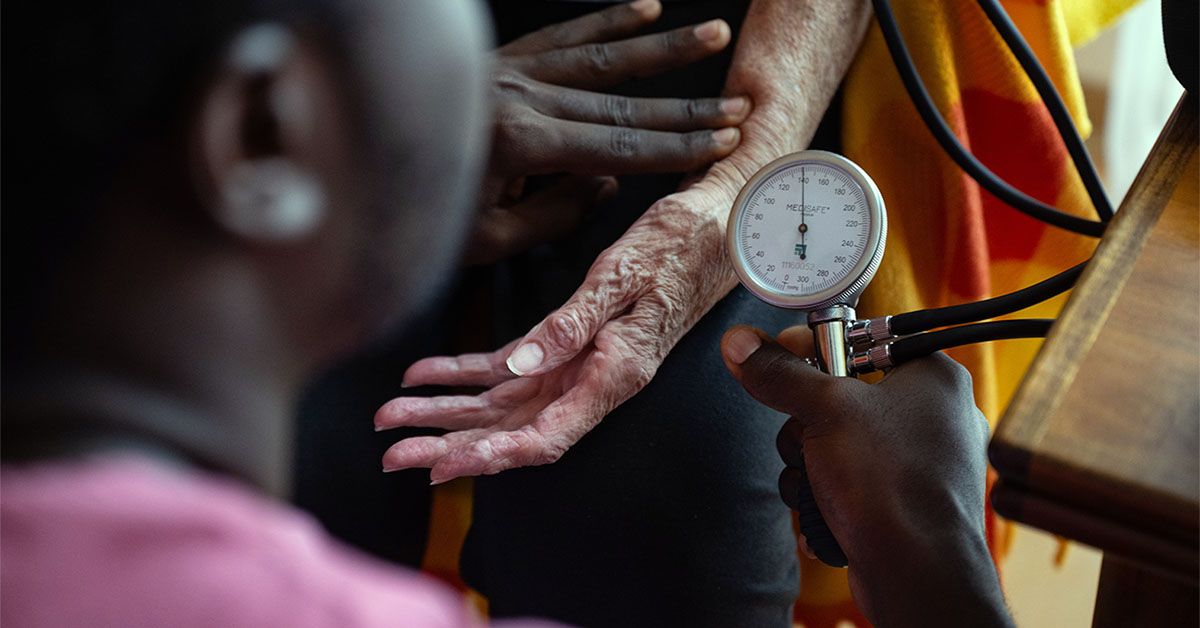
As much as 31% of the world’s population has metabolic syndrome
In a dimly lit café in Stockholm, a group of researchers gathered to discuss alarming new data revealing that nearly one in three adults worldwide grapple with metabolic syndrome. They sipped their coffees with furrowed brows, contemplating the implications of their findings: a stark correlation between this metabolic disorder and the risk of Parkinson’s disease, a life-altering neurodegenerative condition that silently robs individuals of their motor functions. This connection, they agreed, could reshape how we address public health issues linked to metabolic and neurological disorders.
The Hidden Epidemic
Metabolic syndrome—characterized by abdominal obesity, elevated blood sugar, abnormal cholesterol levels, and hypertension—affects an estimated one in four adults globally. But its impact extends well beyond cardiovascular health, planting seeds of concern in the field of neurology. Studies suggest that the risk of developing Parkinson’s disease, which is the second most common neurodegenerative disorder following Alzheimer’s, is significantly heightened for those carrying this syndrome.
A groundbreaking study published in Neurology, the medical journal of the American Academy of Neurology, adds urgency to this conversation. Researchers analyzed medical data from the U.K. Biobank, tracking over 467,000 participants for 15 years. They discovered that 38% of the cohort had metabolic syndrome and, crucially, those affected were approximately 40% more likely to develop Parkinson’s disease compared to their healthier counterparts. This alarming statistic beckons the question: Could managing metabolic syndrome serve as a preventative strategy for one of the most insidious diseases of our time?
Understanding the Connection
“Our findings present metabolic syndrome not just as a risk factor for diabetes and heart disease but as a potential precursor to neurodegenerative diseases like Parkinson’s,” stated Dr. Weili Xu, a prominent researcher associated with the study. She noted that individuals with a genetic predisposition to Parkinson’s could be particularly vulnerable. “It underscores the importance of maintaining metabolic health, especially for those at genetic risk,” she explained.
The Research Findings
- Metabolic Syndrome Definition: Defined as having at least three of the following conditions: abdominal obesity, elevated blood pressure, high blood sugar, and abnormal cholesterol levels.
- Increased Risk: Individuals with metabolic syndrome have a 40% higher probability of developing Parkinson’s disease than those without it.
- Compound Risk: The study also indicated that the presence of genetic markers for Parkinson’s amplifies this risk factor.
The implications are dire. As Dr. Michael S. Okun, director of the Norman Fixel Institute for Neurological Diseases, articulated in a recent interview, “The findings tell us that markers of metabolic health—such as abdominal obesity and abnormal cholesterol—are not mere cardiovascular red flags; they may also accelerate brain neurodegeneration.” He advocates a preventative framework that could redefine how healthcare approaches at-risk populations.
Historical Context and Broader Implications
This new research builds on a growing body of literature linking metabolic syndrome to a variety of serious health conditions, including diabetes, cardiovascular disease, and now, Parkinson’s disease. Dr. Daniel Truong, a neurologist and editor-in-chief of the Journal of Clinical Parkinsonism and Related Disorders, expressed a cautious optimism regarding the findings. “While this evidence is concerning, it strengthens the argument that metabolic syndrome is not merely a vascular or metabolic condition; it’s a systemic disorder with neurological implications,” he explained.
Truong pointed out that Parkinson’s disease often remains undetected for years, allowing it to smolder undiagnosed as early symptoms manifest in non-motor forms such as sleep disturbances or gastrointestinal issues. “Understanding how metabolic conditions contribute to the development of Parkinson’s could allow for earlier interventions and preventative strategies,” he stated, echoing the sentiments of many in the field.
Potential for Intervention
The silver lining in this research is the potential for actionable interventions. With metabolic syndrome being a highly modifiable condition, focusing on lifestyle changes such as weight management, blood pressure control, and blood sugar regulation could have profound implications for public health. Okun emphasizes that addressing these risk factors may one day become a new frontier in Parkinson’s prevention. “We need to explore whether modifying these components can indeed change outcomes,” he noted.
Truong echoed this sentiment, suggesting that healthcare providers should adopt a proactive approach. “In clinical settings, we need to engage patients in discussions about not just their heart health but their brain health, especially if they are presenting with early signs of metabolic syndrome,” he urged. By fostering a public awareness campaign surrounding these interconnected issues, there is hope for averting the upcoming epidemic of neurodegenerative diseases.
A Call for Future Research
This compelling research raises as many questions as it answers. With metabolic syndrome affecting such a large percentage of the global population, the medical community is left pondering: How can we best address this dual crisis of metabolic and neurological health? Further studies and collaborations are crucial for validating these findings across diverse populations and for exploring real-world applications of these interventions.
As the researchers at the café wrapped up their meeting, they acknowledged that while deciphering the complex relationship between metabolic syndrome and Parkinson’s disease presents significant challenges, the stakes have never been higher. The potential for a proactive approach could change the narrative for countless individuals battling neurological illnesses, ensuring that health interventions are rooted in a deeper understanding of the interconnectedness of our bodily systems.
Source: www.medicalnewstoday.com